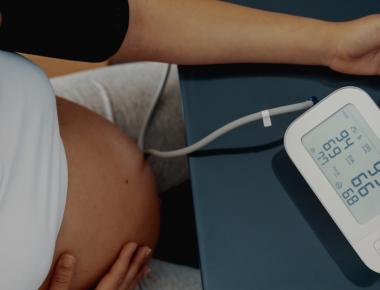
The Effects of Increasing Dialysate Magnesium on Serum Calcification Propensity in Patients with End-Stage Kidney Disease
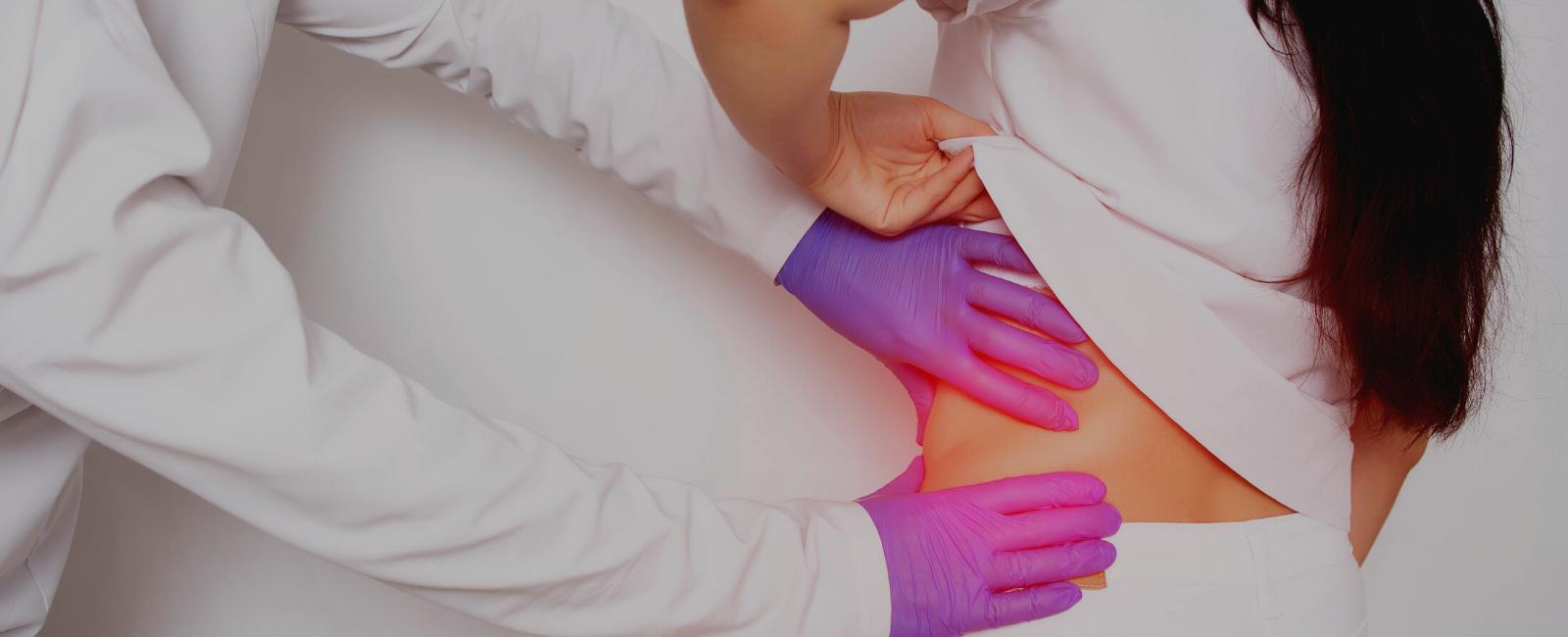
Table Of Contents
The Risk of End-Stage Kidney Disease
Individuals with end-stage kidney disease (ESKD) have a much higher risk of succumbing to a heart attack than the general population, partly because the kidneys help control the calcium levels in the body. When there is a kidney problem, an abnormal calcium build up could occur in the blood vessels, making them stiff and more likely to burst. So, anything that can help keep calcium levels under control may help reduce the risk of heart attacks in people with ESKD.
The Effect of Magnesium on Serum Calcification Propensity (T50)
Vascular calcification is the abnormal buildup of calcium in blood vessels, causing it to harden. It has been shown that secondary calciprotein particles (but not primary calciprotein particles) can cause vascular calcification. Serum calcification propensity (T50) measures how quickly primary calciprotein particles turn into secondary calciprotein particles in serum. A low T50 reflecting an increased calcification propensity is linked with cardiovascular events and all-cause mortality in people with ESKD. Increasing T50 might prevent calcification and reduce the risk of heart problems. Adding magnesium (Mg) to serum increases T50 in a laboratory, so Mg treatment might help improve T50. Increasing the Mg level in a dialysate (fluid composed of water, electrolytes, and salts used during dialysis to remove impurities) is an easy, inexpensive way to increase serum Mg. It might also be effective in increasing T50.
In this randomized, double-blind clinical trial, we tested whether increasing dialysate Mg from 1.0 to 2.0 milliequivalents per liter (mEq/L) for 28 days would increase the T50 of patients with ESKD undergoing maintenance hemodialysis (HD), and that T50 would return to baseline 14 days after returning to standard dialysate Mg.
The Study Method on Increasing Dialysate Magnesium for Serum Calcification Propensity of ESKD Patients
57 subjects completed the study. They were randomized into two groups: 29 received the standard dialysate Mg (1.0 mEq/L) while 28 obtained 2.0 mEq/L dialysate Mg. After the intervention period of 28 days, participants returned to their regular dialysis regimen with standard dialysate Mg of 1.0 mEq/L. They were followed up after 14 days to assess any changes occurring after the intervention.
The Results
In the standard dialysate magnesium group, T50 remained stable. In contrast, a statistically significant increase (that is, improvement) was noted on day seven in the high-dialysate Mg group, and this was sustained for the duration of the intervention. Upon return to dialysate Mg of 1.0 mEq/L, T50 returned to baseline levels in the high-dialysate Mg group.
The Conclusion
The increase in dialysate Mg from 1.0 to 2.0 mEq/L for 28 days significantly increased T50 in subjects with ESKD treated with HD. No incidences of serum Mg greater than 4.4 mg/dl occurred during the trial, and we did not consider any adverse events related to the intervention. Further study is needed to investigate whether increasing dialysate Mg improves clinical outcomes in patients with ESKD.
Reference
Related Posts

Quick Links
Legal Stuff